Keratinocytes
Definition and Location
Keratinocytes represent the major cell type of the epidermis, the outermost of the layers of the skin, making up about 90 percent of the cells there. They originate in the deepest layer of the epidermis, the stratum basale and move up to the final barrier layer of the skin, the stratum corneum. There, keratinocytes are found as nucleus-free, flat, and highly keratinized squamous cells.1
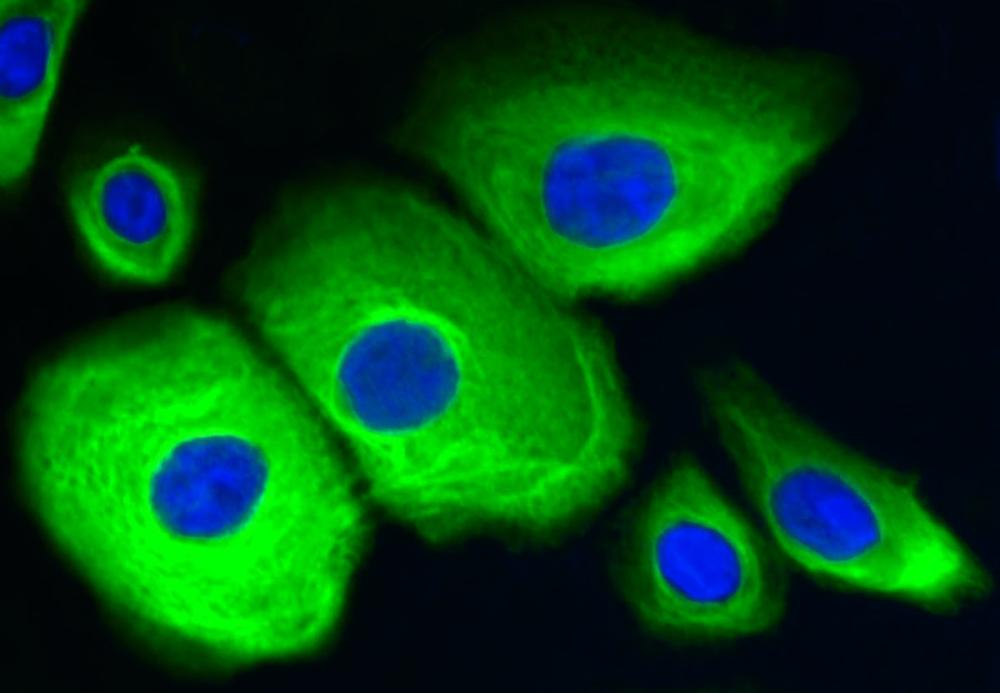

Differentiation of Keratinocytes
Keratinocytes proliferate in the basal layer of the epidermis and start differentiating on their way to the surface, undergoing gradual differentiation. During this process, they profoundly change their morphology and start to produce keratin, cytokines, growth factors, interleukins and complement factors. Keratinocyte differentiation is regulated by several factors as well as by epigenetic regulatory mechanisms.2
Function
Keratinocytes are highly specialized. They play an essential role in protection, as they form a tight barrier that prevents foreign substances from entering the body, while minimizing the loss of moisture, heat, and other constituents. These cells have also a structural role, forming tight bonds with the other cells in the epidermis and maintaining them in their locations. In addition, keratinocytes function as immunomodulators following skin injuries.
Applications
- Keratinocyte Cell Culture
Cultivation of human keratinocytes in monolayer culture was first described by Rheinwald and Green more than 30 years ago. Since then, numerous advances have been made in the cultivation of human keratinocytes, which can be cultured in two-dimensional as well as three-dimensional culture.3 Normal Human Epidermal Keratinocytes (NHEK) can be isolated from juvenile foreskin or from adult normal human tissue from various locations, including face, breast, abdomen, and thighs. For research purposes, NHEK from single donors or pooled donors can be used. The optimal calcium concentration in the culture is essential to ensure the best conditions for both proliferation and differentiation of keratinocytes.
- Characterization
At each stage of differentiation, keratinocytes express specific keratins, but also other markers such as involucrin, loricrin, transglutaminase, filaggrin, and caspase 14.
- Research Applications
Keratinocytes can be used in many applications, such as studies on epidermal development and differentiation, studies on drug uptake, pharmaceutical testing, cosmetic and toxicological testing, and studies on skin aging. They are also used in dermatological research, wound-healing research, and cancer research.
Interactions with other Cells in the Skin
- Keratinocytes and Fibroblasts
The cross-talk between keratinocytes and fibroblasts is essential for maintaining the skin homeostasis and for ensuring a balanced wound-healing process.4 These two cell types communicate through paracrine signaling mechanisms. Disruption of this cross-talk can lead to chronic wounds.
- Keratinocytes and Melanocytes
The interaction of keratinocytes and melanocytes is also crucial for the homeostasis of the epidermis. Melanocytes produce melanin, which absorbs UV waves and prevents DNA damage to the keratinocytes. Keratinocytes, on the other hand, stimulate melanocyte functions such as proliferation, differentiation, and melanogenesis.5
- Keratinocytes and other cells
Keratinocytes have immunomodulatory functions that interact with lymphocytes and Langerhans cells in the skin.
Role in wound healing and inflammation
- Keratinocytes in Wound Healing
Keratinocytes are responsible for restoring the epidermis following injuries.6 This process, called re-epithelialization, is necessary for a successful wound closure. When the skin is injured, keratinocytes become activated and migrate to the wound, where they start proliferating to fill the defect. During wound-healing, interactions between keratinocytes, fibroblasts and immune cells are critical for a successful healing process. Impaired keratinocyte function leads to wound-healing defects and to chronic wounds.
- Keratinocytes in Inflammation
When the epidermal barrier is breached or when pathogens enter the skin, an inflammatory response is triggered. Keratinocytes actively participate in this process, as they express cytokines that transmit positive or negative signals to immune cells.
Keratinocytes play also a role in several allergic skin diseases7, and in chronic inflammatory diseases such as psoriasis, as they can recruit and activate dendritic cells and leukocytes.8
Keratinocytes by PromoCell
The in vitro culture of human skin cells is an essential research tool widely used for assaying dermal toxicity, pharmacological testing, and tissue repair. We offer a comprehensive portfolio of primary human dermal cells including keratinocytes, melanocytes, fibroblasts and hair follicle cells to support these research applications.
Primary Normal Human Epidermal Keratinocytes are available from single or from pooled donors isolated from the epidermis of juvenile foreskin or adult skin from different locations like the face, the breasts, the abdomen, and the thighs. They are the major cell type in the epidermis, making up about 90% of the cells. Additional donor information, like age, sex and skin pigmentation is available for each produced lot.
In addition to cell type-specific marker analysis, each produced lot is tested for growth performance through multiple passages up to 15 population doublings (PD) under culture conditions without antibiotics and antimycotics. In addition, all cells have been tested for the absence of HIV-1, HIV-2, HBV, HCV, HTLV-1, HTLV-2 and microbial contaminants (fungi, bacteria, and mycoplasma).
References
Expand
- Eckert RL, Rorke EA. Molecular biology of keratinocyte differentiation. Environ Health Perspect. 1989 Mar;80:109–116. doi:10.1289/ehp.8980109
- Lee J-H. Keratinocyte Differentiation and Epigenetics. In: Lu Q, Chang CC, Richardson BC, editors. Epigenetics and Dermatology. Academic Press; 2015. p. 37–52. doi:10.1016/B978-0-12-800957-4.00003-5
- Rasmussen C, Thomas‑Virnig C, Allen‑Hoffmann BL. Classical human epidermal keratinocyte cell culture. Methods Mol Biol. 2013;945:161–175. doi:10.1007/978‑1‑62703‑125‑7_11
- Wojtowicz AM, Oliveira S, Carlson MW, Zawadzka A, Rousseau CF, Baksh D. The importance of both fibroblasts and keratinocytes in a bilayered living cellular construct used in wound healing. Wound Repair Regen. 2014 Mar‑Apr;22(2):246–255. doi:10.1111/wrr.12154
- Hirobe T. Keratinocytes regulate the function of melanocytes. Dermatologica Sinica. 2014;32(4):200–204. doi:10.1016/j.dsi.2014.05.002
- Pastar I, Stojadinovic O, Yin NC, Ramirez H, Nusbaum AG, Sawaya A, Patel SB, Khalid L, Isseroff RR, Tomic‑Canic M. Epithelialization in wound healing: a comprehensive review. Adv Wound Care (New Rochelle). 2014 Jul 1;3(7):445–464. doi:10.1089/wound.2013.0473
- Albanesi C, Scarponi C, Giustizieri ML, Girolomoni G. *Keratinocytes in inflammatory skin diseases*. Curr Drug Targets Inflamm Allergy. 2005 Jun;4(3):329–334. doi:10.2174/1568010054022033
- Albanesi C, Madonna S, Gisondi P, Girolomoni G. The interplay between keratinocytes and immune cells in the pathogenesis of psoriasis. Front Immunol. 2018;9:1549. doi:10.3389/fimmu.2018.01549
