Humans can suffer from many different diseases: cancer, diabetes mellitus, atherosclerosis, and viral infections, for example. They affect different types of tissues and lead to a variety of pathophysiologies. But they have one thing in common – a hallmark of those diseases is a dysfunction of the vascular endothelium (Rajendran et al., 2013).
“The vasculature is such a complex system,” explains Professor Simi Ali, a well-respected immunobiologist at the Institute of Cellular Medicine of the Newcastle University in the United Kingdom. “It is important to understand the interactions of endothelial cells among themselves and with the surrounding cells.” The endothelium is the thin layer of endothelial cells (ECs) that lines the interior surface of blood and lymphatic vessels and regulates the functions of the vascular wall. The ECs produce a variety of molecules that are crucial for vascular homeostasis, for local cellular growth, and for inflammatory responses. Endothelial dysfunction is the first step in the pathogenesis of several diseases as atherosclerosis, tumor angiogenesis, metastasis, and transplant rejection (Tan et al., 2004) and is clearly apparent in patients with diabetes (Onat et al., 2011).

Professor Ali investigates the role of chemokines in inflammation, in particular following organ transplantation. “When it comes to transplant rejection, the immune system is involved. Leucocytes pass the endothelial barrier, get to the tissue and cause damage. We want to understand the mechanism of inflammation to be able to block the activation and migration of leukocytes through the vascular wall,” she explains. Her main challenge is finding a robust in vitro model to better understand the pathological processes leading to a breach in the endothelium.
In general, identifying pathological changes in the vascular endothelium before the onset of symptoms could lead to the development of new strategies for risk assessment. Moreover, targeting these processes could prevent or slow down the progression of vascular diseases.
Are HUVECs the best model for your research?
Most research on vascular endothelium uses human umbilical vein endothelial cells (HUVECs). First isolated and cultured in the 70s, HUVECs soon became the mainstay of cell-researcher’s work in many laboratories, as they are readily available, quite easy to culture, highly proliferative, and able to migrate and invade new tissues. However, HUVECs may not be representative of the actual in vivo conditions as they derive from immune-privileged fetal tissue and may differ significantly from adult vascular endothelium. Therefore, results obtained with these cells are often criticized due to the uncertain relevance in adults. “HUVECs do not express some of the adult endothelial markers,” says Professor Ali. “You need to stimulate them with Tumor Necrosis Factor (TNF) to get them to upregulate adhesion molecules, which can then respond to the integrins on leukocytes.”
In recent years, the call for alternatives has grown louder among EC researchers, who were looking for more representative models. “Now the use of primary cells has become more attractive, and there is a vast range of commercially available ECs,” explains Professor Ali. Due to the marked degree of heterogeneity among ECs from different tissues, posing the right question and selecting the right type of cells are crucial for a successful experimental setting. This means that depending on your field of interest, either HUVECs or adult cells might be more suitable. In other words: You now have the agony of choice. Whereas HUVECs provide a very good initial model, adult endothelial cells may be the preferred choice for a better understanding of the tissue-specific dynamics.

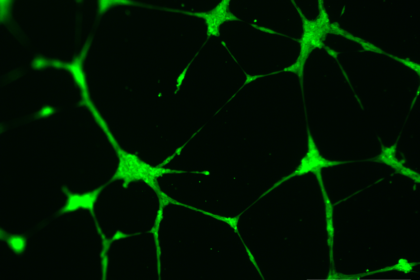
Working with human primary cells is important to mimic the in vivo situation. However, HUVECs do not express all the markers of adult ECs. Picture kindly provided by Professor Simi Ali.
PromoCell offers both HUVECs and a wide spectrum of ECs from large and microvascular vessels in the human body. Cells from large vessels, such as the aorta or saphenous vein, are usually not recommended for studies on neo-angiogenesis, but might be preferable in a study on atherosclerosis, as they display the adult phenotype. Human microvascular ECs (HMVEC) from capillaries, on the other hand, are highly active and best used for researches on neo-angiogenesis in tumors. HMVECs differ in morphology and properties according to the tissues supplied by the capillaries and can be isolated from dermal, lung, cardiac, and uterine tissues, among others.
“When looking for factors that can affect the integrity of the endothelial membrane during inflammation, we first use HUVECs, as they are a very good in vitro model for initial studies,” explains Professor Ali. “Then we use organ-specific primary ECs derived from renal or lung tissue to better understand the mechanisms of transplant rejection. In the future, there might be new experimental models, as we might be able to grow ECs in three dimensions rather than in two.”
Working ex vivo with patients’ Endothelial Cells
For a direct characterization of the phenotype of human ECs, it is necessary to work with primary cells obtained ex vivo through endovascular biopsy. For this purpose, ECs can be isolated from the aorta, from peripheral veins (Onat et al., 2011), and from the saphenous vein (Tan et al., 2004) from healthy patients, as well as from those with vascular diseases. These primary cells offer new perspectives on the human endothelium, as they closely represent their natural environment. However, the limited availability of human endothelial tissue represents a major restriction. Other methods for an ex vivo evaluation of endothelial dysfunction include the quantification of circulating ECs (Boos et al., 2006), endothelial microparticles, (Horstman et al., 2004) or circulating endothelial progenitor cells (Chen et al., 2009).
Having the possibility to choose primary ECs from various origins could take your vascular research to the next level. But you need to make your decision carefully, and know precisely which type of endothelial cell-based methodology comes closest to the in vivo mechanisms in focus. Only if you clearly define the question, will you most likely succeed in answering it.